Ovarian Factor
The two most important variables in female fertility are egg quality and ovulation. Ovulation is the process of releasing the egg from the ovary which may be controlled by many variables.
If the egg is not released, ovulation does not occur and pregnancy cannot be accomplished.
If ovulation occurs, the egg has to be healthy to be fertilized and develop into an embryo in order to implant and result in a healthy pregnancy.
The most common cause of infertility in women of advanced reproductive age is compromised egg quality due to low ovarian (egg) reserve.
At Footsteps To Fertility Centre, we understand that each patient is unique. Every fertility service we offer is customized to you and your unique needs.
No matter how difficult a case, we are driven to help you succeed in your fertility goals.
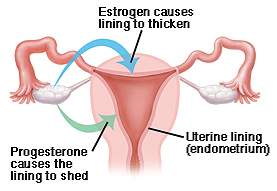
Quizlet. Image source: The Endocrine System and Reproductive System. Accessed via https://quizlet.com/552486168/the-endocrine-system-and-reproductive-system-flash-cards/
Infertility due to a woman’s inability to regularly release eggs, or produce sufficient progesterone, accounts for a significant portion of infertility cases.
Progesterone is a hormone produced by the ovaries that transform the uterine lining allowing a fertilized egg to implant and grow. It is produced only after ovulation.
If you have regular menstrual cycles, you are probably ovulating (releasing ripe eggs from your ovary). If you only have a period every few months or not at all, you are probably not ovulating. Or you may be ovulating infrequently.
By monitoring when you ovulate, you may be able to conceive (become pregnant) more quickly and easily. You can use an over-the-counter ovulation prediction kit. The test kit helps you plan for ovulation before it takes place. That way you can schedule intercourse or insemination at a time when you are most likely to become pregnant.
These urine test kits are designed to detect the surge of luteinizing hormone (LH) that occurs just before you ovulate. The LH surge stimulates one of the ovaries to release an egg and produce progesterone. Ovulation prediction kits usually detect the LH surge about a day or a day and a half before you ovulate.

Egg Quality

Female Egg Quality is synonymous with the probability of embryo implantation. Egg quality refers to the state of an egg as genetically normal or abnormal.
Egg Quality cannot be determined by looking at the egg, measuring its receptivity to fertilization by sperm, or observing initial embryo division. Just because an embryo looks good in the laboratory, does not mean that it will implant.
At Footsteps To Fertility Centre located in Nairobi, Kenya, we are honored to have helped thousands of couples and single mothers receive the gift of parenthood and to be given the opportunity to guide them through their difficult period of infertility.
As you age, the DNA inside your eggs begins to degrade
Because our eggs have been with us since before we were born, they’re exposed to all sorts of damage, but mostly unavoidable, influences throughout our lives: fevers, infections, stress, toxins, free radicals. And because human cells, including eggs, are fragile, this exposure can lead to little “mistakes” in our egg cells’ DNA, called chromosomal abnormalities.
Once a cell’s DNA is degraded, it can’t be fixed medically or “healed.” In other words, once an egg becomes abnormal, it can’t become normal again—egg quality cannot be improved. Egg quality is fairly black-and-white—either an egg is genetically “normal” (euploid) or it’s not (aneuploid), and as women age, a higher and higher percentage of their eggs are abnormal.
Since DNA is like an instruction manual for our cells, any damage to your DNA can prevent that cell from doing what it’s supposed to do—which, in the case of the egg, is to make a healthy baby.
Relationship between Egg Quality And Age
Women’s ovaries are naturally programmed to allow just one egg to grow, mature, and be released (“ovulated”) each cycles (usually each month). That one egg represents the one chance for pregnancy in that particular menstrual cycle.
That egg ovulated may be either normal or abnormal. If it’s normal, great—you have a healthy pregnancy. But if it’s not? Abnormal egg cells typically don’t fertilize or implant in the uterus, but in the rare case they do, they can result in miscarriage or genetic disorders like Down syndrome.
The difference in egg quality between a 25-year-old and a 40-year-old is a matter of the statistical likelihood of the one egg she’s ovulated being normal.
Because women in their late 30s and 40s have a higher percentage of abnormal eggs, it’s much more likely that their one egg each month will be abnormal. That’s why natural fertility declines with age, and why we see infertility, miscarriage, and genetic disorders more often with women over 35.
Bottom line: the age of the egg is the driving force in our chance at pregnancy.
Studies have determined that women doing in vitro fertilization with their own eggs of the same age experience a significant decrease in success rates.
This confirmed an important fact: because age directly correlates with egg quality, and therefore the ability of the egg to fertilize into a healthy pregnancy, it’s the age of the egg that matters most when it comes to fertility.
Yes, there are some risks associated with carrying a pregnancy at what’s called “advanced maternal age” (namely a slightly higher risk of gestational diabetes and preeclampsia), but for the most part, it’s a young, healthy egg that makes for a healthy pregnancy.
That’s why egg freezing works—it allows women to freeze their young, healthy eggs and preserve their egg quality, so they can be their own egg donor later on.
Decreased Ovarian Reserve
OviaHealth. Image source: Pros and cons of freezing your eggs. Accessed via https://www.oviahealth.com/guide/100900/all-about-egg-freezing/
Ovarian reserve refers to the reproductive potential left within a woman’s two ovaries based on the number and quality of eggs. Diminished ovarian reserve is the loss of normal reproductive potential in the ovaries due to a lower count or quality of the remaining eggs. Patients can have diminished ovarian reserve but intact ovarian function.
Normal aging causes most cases of the diminished ovarian reserve but genetic defects, aggressive medical treatments that harm the reproductive system (radiation for cancer), some surgeries and injury can cause DOR as well. In many cases, there is no apparent cause for a relative decrease in ovarian reserve.
At Footsteps To Fertility located in Nairobi, Kenya, a routine part of the infertility evaluation includes comprehensive testing for ovarian reserve in order to determine a treatment course and to predict the likelihood of pregnancy with any specific treatment protocol. Our goal is to increase egg quality, health and responsiveness which in turn will increase the health of developing embryos.
Women diagnosed with diminished ovarian reserve have the same reduced success of conceiving with in vitro fertilization (IVF) as they do with natural efforts to conceive. In addition, women with DOR often have a greater risk of miscarriage when conceiving via IVF with their own eggs due to lower egg quality.
Ovarian reserve can also be considered a part of the biological clock, but this clock can vary from woman to woman. Some women continue to be fertile in their 40s, while others begin to lose their fertility in their 20s. Women are born with around 2,000,000 eggs, which is all the eggs they’ll ever have.
Eggs are continuously lost, so by the onset of puberty, most women have around 500,000 eggs left. By a woman’s late 30s this number will have further declined to around 27,000. At the onset of menopause, most women only have around 1,000 eggs left in their ovaries.
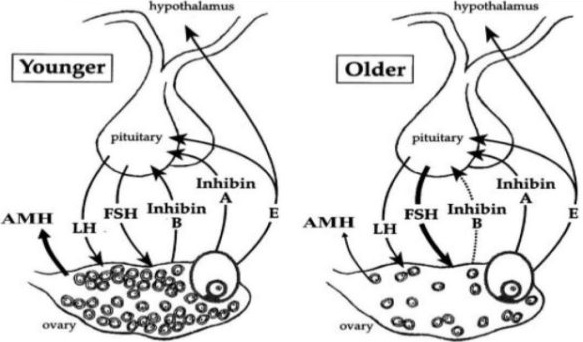
Science Direct. Image source: Inhibin and reproductive aging in women. Accessed via https://www.sciencedirect.com/science/article/abs/pii/S0378512298000747
Our team at Footsteps To Fertility located in Nairobi, Kenya strives to provide you with exceptional support services through our Patient Services Team, and offer customized fertility care packages which can be bundled with medication and genetic testing services.
The main causes of decreased ovarian reserve are:
- Cigarette smoking.
- Genetic abnormalities (Fragile X and other X chromosome abnormalities).
- Aggressive treatments (radiation for cancer).
- Ovarian surgery, such as for endometriosis.
- Idiopathic (this means that there is no apparent cause).

Diagnosis of DOR
Decreased ovarian reserve presents no symptoms in most women. Some women may see a shortened menstrual cycle, such as from 28 days to 25 days. But for the most part, women find out they have DOR after diagnostic testing.
These include transvaginal ultrasound and hormone evaluations for follicle-stimulating hormone (FSH), estradiol (a form of estrogen) and the anti-Müllerian hormone (AMH).
FSH and estrogen are good indicators of fertility, as well as of a woman’s response to ovulation induction or stimulation, which can help her conceive.
The anti-Müllerian hormone usually correlates well with fertility potential by reflecting the number of eggs left in the body.
These two hormone level tests, combined with a transvaginal ultrasound, can detect diminished ovarian reserve with a high level of certainty.
Fertility treatments women with DOR
No treatments can slow ovarian aging and truly prevent diminished ovarian reserve. However, women with DOR who still want to conceive have options through assisted reproductive technologies.
When a woman is diagnosed with diminished ovarian reserve, she can take an immediate step and try fertility preservation. Fertility preservation involves retrieving a woman’s eggs from her ovaries and freezing them for later use.
The best time for women to freeze eggs is when they are young and their ovarian reserve is better.
Women can also use ovarian superovulation, which is an exaggerated form of ovulation induction. This treatment uses injectable hormones to induce the woman to ovulate multiple eggs. The eggs are then collected for cryopreservation or for use in a fresh IVF cycle to create an embryo and implant it in the woman’s womb.
Donor eggs in conjunction with IVF are often the best option for women with a low ovarian reserve, especially if their remaining eggs are of low quality. A woman can achieve pregnancy using the donor eggs fertilized by her partner’s sperm (or donated sperm) and having the resulting embryo implanted in her uterus.
Although the resulting child will not have the birth mother’s genes (but will have the genes of the egg donor and the partner’s or donated sperm), the recipient mother gets to carry a pregnancy to term and give birth.
Absence of Menses

When you miss your period, the doctor calls this condition amenorrhea. Since there are many possible reasons for this symptom, your doctor will have to do a detailed evaluation to come to the right diagnosis.
Sometimes there is the absence of a menstrual period in a woman of reproductive age. Physiological states of the absence of menstruation are seen, most commonly, during pregnancy and lactation (breastfeeding), the latter also forming the basis of a form of contraception known as the lactational amenorrhoea method.
Amenorrhea is the medical term that is used to describe the absence of periods. Remember that amenorrhea itself is not a disease, but is usually a symptom of another condition.
Depending on the reason, you might experience other symptoms, such as headache, vision changes, milky nipple discharge, hair loss, or excess facial hair.
Doctors classify amenorrhea as being either physiologic or pathologic (abnormal). Women normally do not menstruate before puberty, during pregnancy, and after menopause – these are the physiological causes of amenorrhea. However, if a woman does not get her period when she normally should, it may be the symptom of a medical condition.
At Footsteps To Fertility Centre located in Nairobi, Kenya, our experienced team will provide support, diagnosis and effective treatment for the absence of menses so as to get you back to your quality health.
Types of Amenorrhea
At Footsteps To Fertility Centre located in Nairobi, Kenya, we are honored to have helped thousands of couples and single mothers receive the gift of parenthood and to be given the opportunity to guide them through their difficult period of infertility.
There are two types of Amenorrhea. They include;
- Primary amenorrhea is when a young woman has not had her first period by the age of 16.
- Secondary amenorrhea is when a woman who has had normal menstrual cycles stops getting her monthly period for three or more months.
What Causes Amenorrhea?
Amenorrhea can be caused by anything which affects the normal functioning of the organs and hormones involved in menstruation. Since menstruation is such a complex process, it’s not surprising that a large number of conditions could cause amenorrhea.
Possible causes of primary amenorrhea (when a woman never gets her first period) include:
- Failure of the ovaries. This is called POF, or premature ovarian failure
- Problems in the central nervous system (brain ) or the pituitary gland, which cause hypogonadotropic hypogonadism
- Absent uterus (Mullerian agenesis)
Common causes of secondary amenorrhea (when a woman who has had normal periods stops getting them) include:
- Pregnancy
- Anovulation, often because of PCOD
- High prolactin levels (hyperprolactinemia)
- Ovarian failure (premature menopause)
- Functional ovarian cysts
- Drugs and medicines
- Stress and depression
- Poor nutrition
- Certain drugs, such as antipsychotics and antidepressants
- Extreme weight loss (anorexia)
- Over-exercising can cause athletic (hypothalamic) amenorrhea
- Ongoing systemic illness
- Thyroid gland disorders – both an overactive (hyperthyroidism) or underactive (hypothyroidism) thyroid gland can cause menstrual irregularities, including amenorrhea. Intrauterine adhesions (Asherman syndrome).
Diagnosis For Amenorrhea
The commonest reason for missing a period in infertile women is anovulation.
The list of causes looks very intimidating, and you may be completely confused as to what the possible diagnosis in your case is. However, let me try to simplify this, so it’s easier for you to make sense of what the doctor will do.
Let’s start with the basics. In order to get a period, you basically need just two things:
- a uterus, which sheds its uterine lining as a period
- hormones ( estrogen and progesterone) which act on the uterine lining, and cause it to shed
If you miss a period, this means there are only 2 broad possibilities.
- There’s a problem with the uterus. Thus, maybe damaged ( because of intrauterine adhesions)
- There’s a problem with the reproductive hormones. Their levels may be too low; or too high, or out of balance
The first test the doctor may do is a vaginal ultrasound scan to check your uterus; and your uterine lining. If this is normal, then it’s likely the problem is with your hormones.
Sometimes, the doctor may give you hormones as a therapeutic trial to see if this can induce your period. This is called a progesterone challenge test; and consists of 5 days of 20 mg medroxyprogesterone daily. Thus, if you get your periods after taking progesterone, this means your uterus is fine; that you have high estrogen levels; and that you are not producing progesterone on your own (this is the picture classically found in women with PCOD).
If you do not get your periods after taking the progesterone, this means either that your uterus is damaged; or that you are not producing enough estrogen.
The other possibilities include: pregnancy; and the possibility of a functional ovarian cyst ( which can produce estrogen and progesterone and delay the period)
If you miss your periods, your doctor will have to run tests in order to find out what the problem is. If you keep an accurate menstrual diary, this will help the doctor in making the right diagnosis. When was your last period? Was it normal? What were your periods like before this?
Treatment For Absence of Menses
The treatment depends on the cause of your amenorrhea. Options for treatment include:
- Medicines that help control abnormal hormone levels
- Surgery for tumors of the pituitary, ovaries, or adrenal glands
- Counseling about how to eat a balanced diet, keep a healthy weight, and cope with stress.
Your doctor might also prescribe estrogen therapy to relieve hot flashes and vaginal dryness and to protect your bones. Calcium and vitamin D supplements, along with strength training, also help keep your bones strong. If you are trying to get pregnant, other treatments might be needed.
Book Your
Appointment today!
Make an Appointment


